Influenza and Covid-19: when vaccination campaigns overlap
November 30, 2021
Background
Without fully capping off one vaccination campaign, Canada has jumped into another. Just a few months after the rollout of mass COVID-19 vaccinations, Canadian provinces are now multiplying efforts to distribute flu shots. Some provinces like British Columbia and Ontario have even expanded their usual programs and now offer free-of-charge flu vaccines to everyone, not only at-risk populations as it has been in past years. This increased public insistence on the flu vaccination campaign is directly linked to the Covid-19 pandemic. Last year’s social distancing measures almost eradicated the flu completely in Canada, which practically means that Canadians currently have lower immunity against newly circulating influenza strains than usual. Under these conditions, the threat of COVID-19 is even more potent; individuals now risk contracting both diseases at the same time, increasing their risk for more serious symptoms, and the combination of hospitalizations for serious flu, COVID-19 and comorbid cases could easily overwhelm healthcare systems. Health officials are thus highly concerned about Canada’s 2021 epidemiological landscape, and working hard to prevent an escalation of flu cases.
Want more information? Interested in engaging us in a research project? Reach out!
Public perceptions of the need, safety and desirability of obtaining a flu shot in Canada though are currently unknown. Heightened saliency of vaccination issues and general health concerns during the pandemic could both benefit and challenge a flu vaccination campaign. On the one hand, increased awareness around the role and importance of vaccination on public health as a result of the pandemic could increase vaccination rates and lead some to opt for a flu shot for the first time. On the other hand, Canadians vaccinated against COVID-19 could feel a false sense of security linked to their vaccination status, feel that they have done enough to protect themselves and others this year, or fear similar side effects as what they might have experienced with the COVID-19 vaccine, and ultimately hesitate about the necessity or advantage of getting a flu shot. Finally, the anti-vaccination movement has gained a greater foothold in the Canadian consciousness as a result of public discourse during the pandemic, which may decrease the desire to get a vaccination of any kind for some. At this moment in time, it is unclear if motivations exceed barriers, and whether the pandemic might impact the flu season and vaccination.
Method
DataSciences conducted an online survey among a representative sample of Canadians (N=1,180) from OCT 29 to NOV 8, 2021, while the flu vaccination period was in full swing. In order to investigate motivations and barriers to flu vaccination in 2021, we inquired about Canadians’ willingness to take the flu shot and the motivations behind their decision. Survey data was weighted by gender, age and region to be representative of the Canadian population. The margin of error for a probabilistic sample of the same size is ± 3.09%.
Openness to vaccines extend beyond the targeted disease
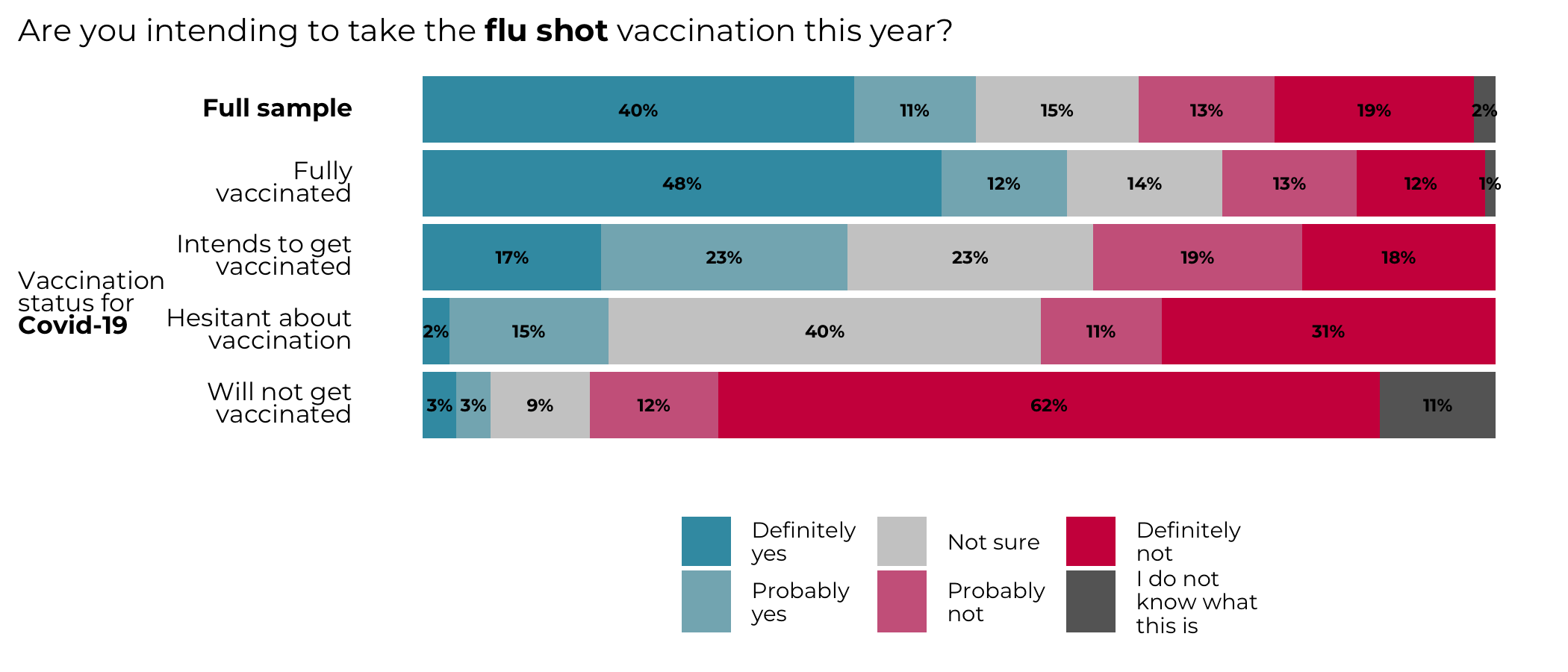
40% of respondents say that they ‘definitely’ intend to take the flu shot in 2021. Although survey numbers could be inflated by social desirability biases, this number is in line with results from previous vaccination campaigns in 2018 and 2019. Intent to take the flu shot is strongly correlated with self-declared COVID-19 vaccination status; while most fully vaccinated Canadians say they will definitely or probably take the flu shot (60%), 62% of respondents who do not intend to get vaccinated against COVID-19 similarly declare that they will definitely not take the flu shot. Individuals who are not vaccinated against COVID-19 represent 11% of our sample. Respondents over 65 years old (61%) and those living in Western Canada (BC: 47%, Prairies: 49%, Alberta: 44%) were the most likely to say they would definitely take the flu shot.
At first glance, it does not seem like our experience with COVID-19 will increase vaccination rates: 69% of respondents who said they would ‘definitely’ get a flu shot also said they take this shot every year, and those who say they will ‘probably’ get one tend to get a shot most years (42%) or every year (19%). However, the pandemic may have heightened the need for extra protection for Canadians between 50 and 64; this age group was overrepresented in first-time flu shot vaccines.
Canadians rated a desire to ‘protect others’ as the most important motivation underlying their decision to take the flu shot: 68% say that this is a ‘very important’ factor in their decision. A majority of those intending to get the flu shot also cite a desire to increase one’s immunity, decrease pressure on the healthcare system, and avoid displaying COVID-19-like symptoms in public as important reasons to get the shot as well. Older respondents tend to be less concerned about having flu symptoms that could be misinterpreted by others than younger respondents, while men also care less about this than women.
Those who said that they will not get a shot reported myriad different reasons. . Lack of concern for contracting the virus (25%) or a perceived low likelihood to give it to others (22%) were most commonly cited. 22% said that having had ‘enough vaccines this year’ is a very important reason for them, but more – 38% – said this is not at all a factor behind their decision. 19% of respondents who refuse the flu shot say being unsure about vaccine safety, in general, is a very important season to not get vaccinated. However, it is unlikely that these respondents would have gotten the flu shot had it not been for COVID-19; among them, only 7% say that they receive a flu shot every year or most years, and half of them (51%) have never received a single flu shot.
If not COVID-19, what motivates people to get flu shots?
Openness towards COVID-19 and flu vaccines are strongly correlated, but the specific context of the pandemic does not seem to be the primary driver or barrier to flu shot vaccination, more than the concern or lack thereof of contracting influenza.
Which other factors might impact one’s likelihood to respond positively to flu shot vaccination campaigns?
- Respondents who are unwilling to take a flu shot score significantly higher than others on anti-intellectualism (+13%), a concept that measures distrust in experts and scientific facts including those related to vaccination. Typically individuals who have studied science at a higher level have greater trust in the scientific method, which can be crudely measured by educational attainment. We found an expected relation between educational attainment and openness to flu vaccines as well; according to our results, 55% of Canadians with a high school degree or lower say they would definitely or probably take a flu shot, compared to upwards of 65% of those with university degrees. These findings warrant the need to educate Canadians from an early age about the role of vaccination on public health and to vulgarize scientific concepts, in order to build trust in experts and science over time.
- Willingness to take a flu shot is also correlated with income: those who do not consider taking the flu vaccine report an average income of $47,750, compared to $58,250 among respondents who say they will take the flu shot. This suggests that extending in the long term outreach strategies initiated because of the pandemic context, such expanding the gratuity of the flu shot, could be effective to ensure a strong vaccination coverage across groups.
Conclusion
On the whole, the pandemic and COVID-19 do not seem to have dramatically shifted the way most Canadians think about vaccines for the flu. If anything, greater saliency about the issues surrounding vaccination may simply intensify hesitancy among those already hesitant, and uptake among those already likely to get vaccinated. At this moment, our data does not predict greater vaccination rates against the flu than in previous years nor an influx of first-time flu shot takers, with one exception: we may see a proportionally higher number of men and women between 50-64 opting for a flu vaccine for the first time, likely due to perceived greater risk among this group to COVID-19 complications from comorbidity.
Our results do suggest potential angles for public health campaigns. These campaigns are likely to be most effective if they align with core values or provide information that can tap into other core motivations, such as self-protection and the protection of others. As such, campaigns should remind audiences of their desire to protect others and may educate them about the public’s lessened immunity in 2021.
Finally, our data is just a snapshot in time, and behavioural intentions are generally found to only predict actual behaviour 28% or so of the time. Ultimately, our data also indicates that new factors are in play for the first time – young people are more self-conscious than ever about exhibiting flu symptoms in public, healthcare systems are already under extraordinary pressures, and travel is back on the rise in a high-disease threat environment – so time will tell how the pandemic has really impacted our relationship with vaccination in general.
Want more information? Interested in engaging us in a research project? Reach out!


